OCCUPATIONAL STRESS, MENTAL HEALTH AND IT’S CORRELATES AMONG HEALTHCARE WORKERS IN AHMADU BELLO UNIVERSITY TEACHING HOSPITAL, ZARIA, KADUNA STATE- NIGERIA
DOI:
https://doi.org/10.33003/fjs-2026-1003-4769Keywords:
Occupational stress, mental health, healthcare workers, job satisfaction, hospital-based studyAbstract
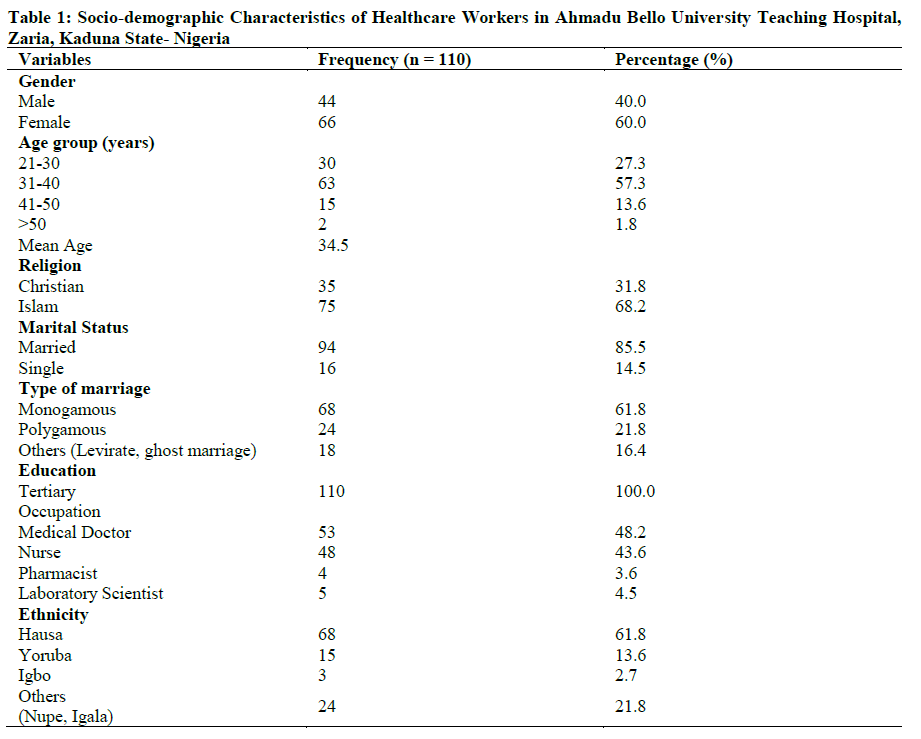
Healthcare workers (HCWs) face increasing occupational stress and poor mental health outcomes due to high workloads, long shifts, and resource constraints. This study assessed occupational stress, mental health, and their correlates among HCWs in Ahmadu Bello University Teaching Hospital (ABUTH), Zaria, Nigeria. A hospital-based cross-sectional study was conducted among 110 HCWs (53 doctors, 48 nurses, 4 pharmacists, and 5 laboratory scientists). Participants were selected using proportional sampling. Data were collected using a structured, interviewer-administered questionnaire incorporating the Brief Job Stress Questionnaire (BJSQ) and the General Health Questionnaire (GHQ-28). Respondents had a mean age of 34.5 years; 60% were female. Mental stress was prevalent, with 50.9% reporting sleep loss due to worry and 42.7% experiencing nervousness. Overall, 57.3% of HCWs reported work-related stress. Age (χ² = 12.34, df = 3, p = 0.015) and gender (χ² = 4.22, df = 1, p = 0.04) were significantly associated with mental stress. A positive correlation was observed between occupational stress and mental health problems (r = 0.56, p = 0.001), while job satisfaction negatively correlated with stress (r = -0.40, p = 0.021). This occupational stress is significantly associated with poor mental health among HCWs in ABUTH. Workload and low job satisfaction are key drivers. Interventions to reduce workload, improve job satisfaction, and provide mental health support are essential to safeguarding HCWs’ wellbeing.
References
Abubakar, A. K., Yisa, M. N., and Olukorode, S. O. (2025). Prevalence of mental health illness in Nigeria: Protocol for a systematic review and meta-analysis. Systematic Reviews, 14,180.
AbuRuz, M. E. (2014). A comparative study about the impact of stress on job satisfaction between Jordanian and Saudi nurses. European Scientific Journal, 10(17), 1857–7881.
Angioha, P. U., Omang, T. A., Ishie, E. U., & Iji, M. E. (2020). Employee stressors and wellbeing of healthcare workers in government-owned hospitals in Calabar, Nigeria. Journal of Public Administration, 2(4), 2020.
Etim, J. J., Bassey, P. E., Ndep, A. O., Iyam, M. A., & Nwikekii, C. N. (2015). Work-related stress among healthcare workers in Ugep, Cross River State, Nigeria. International Journal of Public Health, Pharmacy and Pharmacology, 1(1), 23–34.
Girma, S., Mohammed, A., & Tesfaye, M. (2021). Prevalence of occupational stress and associated factors among healthcare professionals in Ethiopia. BMC Public Health, 21(1), 1–10. https://doi.org/10.1186/s12889-021-11977-3
Nabirye, R. C., Brown, K. C., Pryor, E. R., & Maples, E. H. (2011). Occupational stress, job satisfaction and job performance among hospital nurses in Kampala, Uganda. Journal of Nursing Management, 19(6), 760–768. https://doi.org/10.1111/j.1365-2834.2011.01240.x
NIOSH. (2006). Work organization and stress. World Health Organization.
Pappa, S., Ntella, V., Giannakas, T., Giannakoulis, V. G., Papoutsi, E., & Katsaounou, P. (2020). Prevalence of depression, anxiety, and insomnia among healthcare workers during the COVID-19 pandemic: A systematic review and meta-analysis. Brain, Behavior, and Immunity, 88, 901–907. https://doi.org/10.1016/j.bbi.2020.05.026
Sasaki, N., Asaoka, H., Kuroda, R., Tsuno, K., Imamura, K., & Kawakami, N. (2021). Sustained poor mental health among healthcare workers in COVID-19 pandemic: A longitudinal analysis. Journal of Occupational Health, 63(1), e12227. https://doi.org/10.1002/1348-9585.12227
1 CDCP. (2020). Centre for Disease Control and Prevention. Stress at work https://www.cdc.gov/niosh/docs/99-101/default.html
2 Kakemam, E. Raeissi, P. and Raoofi, S. (2019). Occupational stress and associated risk factors among nurses: a cross-sectional study. Contempt Nurse; 55:237–49.
4 Zhang, X. Zhao, K. and Zhang, G. (2020). Occupational Stress and Mental Health: A Comparison between Frontline Medical Staff and Nonfrontline Medical Staff during the 2019 Novel Coronavirus Disease Outbreak. Front Psychiatry; 11:555703.
6 Nguyen-Ngoc, A. Le Thi Thanh, X. and Le Thi, H. (2019). Occupational stress among health worker in a national Dermatology hospital in Vietnam. Front Psychiatry 2018; 10: https://www.frontiersin.org/articles/10.3389/fpsyt.2019.00950/full
7 Williams, E. S. Manwell, L. B. and Konrad, T. R. (2007). The relationship of organizational culture, stress, satisfaction, and burnout with physician-reported error and suboptimal patient care: results from the MEMO study. Health Care Manage; 32:203–12.
8 Lee, I. and Wang, H. H. (2002). Perceived occupational stress and related factors in public health nurses. Journal of Nurse Research; 10:253–60.
9 Teraoka, M.and Kyougoku, M. (2019). Structural relationships among occupational dysfunction, stress coping, and occupational participation for healthcare workers. Work Order Record; 64:833–41.
10 Prins, J. T. Gazendam-Donofrio, S. M. and Tubben, B. (2007). Burnout in medical residents: a review. Medical Education; 41:788–800.
11 Ribeiro, R. P. Marziale, M. H. P. and Martins, J. T. (2018). Occupational stress among health workers of a university hospital. Revista Gaúcha de Enfermagem; 39:S1983-14472018000100421.
12 Low, Z. X. Yeo, K. A. and Sharma, V. K. (2019). Prevalence of Burnout in Medical and Surgical Residents: A Meta-Analysis. International journal of Environmental Research; Public Health; 16:1479.
19 Salam. (2020). A. Job stress and job satisfaction among health care professionals. Qatar Foundation Annual Research Conference Proceedings; :HBOP2571Qatar National Convention Center (QNCC), Doha, Qatar.
20 Bhatia, N. (2010). Occupational Stress Amongst Nurses from Two Tertiary Care Hospitals in Delhi.:731–8.10.4066http://www.amj.net.au/index.php?journal=AMJ&page= article&op=viewFile&path%5B%5D=289&path%5B%5D=681
21 Mehta, R. K. and Singh, I. K. (2014). Stress among nurses working in critical care areas at a tertiary care teaching hospital, Nepal. Journal of Chitwan Medical Colloge; 4:42–8.
22 Kshatri, J. S. Das, S. and Kar, P. (2017). Stress among Clinical Resident Doctors of Odisha: A Multi-Centric Mixed Methodology Study. International Journal of Public Health Research and Development; 8:122.
12. Brunner, B. Igic, I. Keller, A. C. and Wieser, S. (2019). Who gains the most from improving working conditions? Health-related absenteeism and presenteeism due to stress at work. European Journal of Health Economics. 20:1165–1180. doi: 10.1007/s10198-019-01084-9.
Jonghee, C. Jin-Hyo, K. Jae, Y. L. Hee, S. K. Dong-wook, L. Yun-Chul, H. Mo-Yeol, K. (2022). The association between occupational stress level and health-related productivity loss among Korean employees; pidemiol Health; 45:e2023009. doi: 10.4178/epih.e2023009
Gebeyehu, S. and Zeleke, B. (2019). Workplace stress and associated factors among healthcare professionals working in public health care facilities in Bahir Dar City, Northwest Ethiopia, 2017. Research Notes; 12:249.
Downloads
Published
Issue
Section
Categories
License
Copyright (c) 2026 Hamza Isa, Zakiyya Hamza, Hassan Shehu Mohammed, Haruna Abdullahi

This work is licensed under a Creative Commons Attribution 4.0 International License.




