HEALTH SYSTEM UNDER PRESSURE ASSESSING THE IMPACTS OF FUNDING VOLATILITY ON MATERNAL, CHILD, AND INFECTIOUS DISEASE SERVICES IN NIGERIA
DOI:
https://doi.org/10.33003/fjs-2026-1005-4920Keywords:
Health Financing, Health Systems, Child and Maternal DeathAbstract
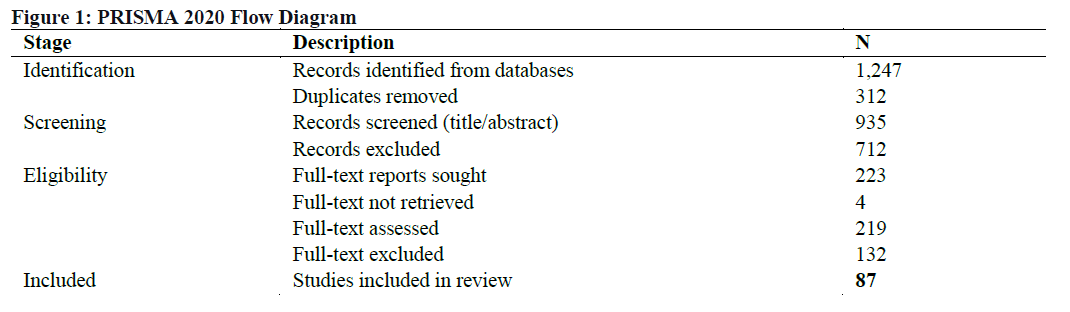
Nigeria's health system faces chronic funding instability; however, the impact of financing volatility on service delivery failures remains poorly understood. This systematic review examines the impact of funding volatility on maternal, child, and infectious disease services in Nigeria. Following PRISMA guidelines, we searched PubMed, Scopus, Web of Science, and institutional repositories for literature published between 2010 and 2026. From 1,247 initial records, 87 studies met the inclusion criteria. An integrated theoretical framework combining the WHO Health System Building Blocks and Health Financing Functions guided the analysis. Financing volatility operates through three mechanisms: revenue collection inadequacy with government spending below one percent of GDP, pooling fragmentation with out-of-pocket payments exceeding seventy percent of health expenditure, and purchasing inefficiency characterized by delayed budget releases. These cascade through the health system, producing medicine stock-outs in sixty-eight percent of facilities, health worker demoralization contributing to forty-five percent attrition in some areas, and catastrophic household expenditure affecting fifteen to twenty-five percent of families. Policy responses, for instance, the Basic Health Care Provision Funds, were affected by political economy constraints and governance fragmentation. Financing volatility fundamentally drives health system fragility in Nigeria. The study recommended to meet the 15% Abuja Declaration health funding target; subsidize insurance for pregnant women, children, and the poor; and require 40% female representation on facility committees and report equity-disaggregated data.
References
Abubakar I, Dalglish SL, Angell B, Sanuade O, … et al. (2022). The Lancet Nigeria Commission: Investing in health and the future of the nation. The Lancet 19; 399(10330):1155-1200. doi: 10.1016/S0140-6736(21)02488-0. PMID: 35303470; PMCID: PMC8943278.Adie, A. E., Tina, A. W., Ineyekineye, A., Eze, V. H. U., & Onongha, C. (2025). Building a Resilient Health System in Nigeria: Strategies, Empirical Evidence, and Policy Recommendations for Sustainable Healthcare Development. Journal of Scientific and Experimental Sciences, 5(1), 1-8. Doi:10.59298/RIJSES/2025/511800Adomi, S., Asogun, D., Rwuaan, R. K., Iliya, B. T., & Adebanjo, O. (2024). Equity of healthcareAccess in Nigeria: A scoping review. The Nigerian Health Journal, 24(3), 1345–1354.DOI: https://doi.org/10.60787/tnhj.v24i3.891Arhin, K., Oteng-Abayie, E. F., & Novignon, J. (2023). Effects of healthcare financing policy tools on health system efficiency: Evidence from sub-Saharan Africa. Heliyon, 9(10), e20573.doi: 10.1016/j.heliyon.2023.e20573. PMID: 37860558; PMCID: PMC10582374Awoyemi, B. O., Makanju, A. A., Mpapalika, J., & Ekpeyo, R. S. (2023). A time series analysis of government expenditure and health outcomes in Nigeria. Journal of Public Health in Africa, 14(7), 1409.doi: 10.4081/jphia.2023.1409. PMID: 37680869; PMCID: PMC10481895.Baker, D. W. (2024). Achieving health care equity requires a systems approach. The Joint Commission Journal on Quality and Patient Safety, 50(1), 1–5.doi: 10.1016/j.jcjq.2023.10.018Burau, V., Falkenbach, M., Neri, S., Peckham, S., Wallenburg, I., & Kuhlmann, E. (2022). Health System resilience and health workforce capacities: comparing health system responses during the COVID‐19 pandemic in six European countries. The International Journal of Health Planning and Management, 37(4), 2032–2048.doi: 10.1002/hpm.3446. PMID: 35194831; PMCID: PMC9087528.Chao, J. (2024). Health Policy: Implementation Challenges, Societal Impact, and Strategic Approaches for Effective Governance. Journal of Pharmaceutical Care and Health Systems, 11(4), 334. DOI: 10.35248/2376-0419.24.11.334Chen, A. M. (2025). Practical barriers to health equity: Challenges, opportunities, and solutions. Advances in Public Health, 2025, Article 2257356.https://doi.org/10.1155/adph/2257356Chukwuma, A. and Obi, F.A. (2025). A Political Economy Analysis of Health policymaking in Nigeria: The Geneis of the 2014 National Health Act.Health Policy and Planning 40 (1)459 – 470. Doi:10.1093/heapol/czaf007.Croke, K., & Ogbuoji, O. (2024). Health reform in Nigeria: the politics of primary health care and Universal health coverage. Health Policy and Planning, 39(1), 22–31.doi: 10.1093/heapol/czad107. PMID: 37978878; PMCID: PMC10775211.Cunningham, R., Polomano, R. C., Wood, R. M., & Aysola, J. (2022). Health systems and health Equity: Advancing the agenda. Nursing Outlook, 70(6, Suppl 1), S66–S76.doi: 10.1016/j.outlook.2022.05.010. PMID: 36446541.Dan-Nwafor C, Ochu CL, Elimian K, Oladejo J, et al. (2020). Nigeria's public health response to The COVID-19 pandemic: Journal of Global Health 10(2):020399. doi: 10.7189/jogh.10.020399. PMID: 33274062; PMCID: PMC7696244.Dsouza SM, Katyal A, Kalaskar S, Kabeer M, Rewaria L, Satyanarayana S, Nallamalla, K.R.&Maulik Chokshi, M. (2024). A scoping review of health systems resilience assessment frameworks. PLOS Glob Public Health 4(9): e0003658. https://doi.org/10.1371/journal.pgph.0003658Gabani J, Mazumdar S, Suhrcke M. (2022). The effect of health financing systems on health System outcomes: A cross-country panel analysis. Health Economics 32(3):574-619. doi: 10.1002/hec.4635. PMID: 36480236; PMCID: PMC10107855.Gilson, L., Barasa, E., Nxumalo, N., Cleary, S., Goudge, J., Molyneux, S., Tsofa, B., & Lehmann, U. (2017). Everyday Resilience in District Health Systems: Emerging Insights From the Front Lines in Kenya and South Africa. BMJ Global Health, 2 (2) e000224.https://doi.org/10.1136/bmjgh-2016-000224Hafez, R. (2018). Nigeria Health Financing System Assessment. Health, Nutrition and Population Discussion Paper. World Bank. Retrieved from https://documents1.worldbank.org/curated/en/782821529683086336/pdf/127519-WP-PUBLIC-add-series-NigeriaHFSAFINAL.pdf on 12th February, 2026.Human Rights Watch. (2025). New Data Exposes Global Healthcare Funding Inequalities.Retrieved from https://www.hrw.org/news/2025/04/10/new-data-exposes-global-healthcare-funding-inequalities on 12th February, 2026.Jindal, M., Chaiyachati, K. H., Fung, V., Manson, S. M., & Mortensen, K. (2023). Eliminating health care inequities through strengthening access to care. Health Services Research, 58(Suppl 3), 300–310. doi: 10.1111/1475-6773.14202. PMID: 38015865; PMCID: PMC10684044.Josiah BO, Enebeli EC, Duncan BA, Adejumo PO, … et al. (2025). Critical review of healthcare Financing and a survey of system quality perception among healthcare users in Nigeria (2010-2023). PLOS Glob Public Health. 5(5):e0004615. doi: 10.1371/journal.pgph.0004615. PMID: 40435126; PMCID: PMC12118842.Kagwanja N, Waithaka D, Nzinga J, Tsofa B, Boga M, Leli H, Mataza C, Gilson L, Molyneux S, Barasa E. (2020). Shocks, stress and everyday health system resilience: experiences from the Kenyan coast. Health Policy Plan. 35(5):522-535. doi: 10.1093/heapol/czaa002. PMID: 32101609; PMCID: PMC7225571.Kakade, S. V., Suke, S. P., Patil, D., Ali, G. S., Garud, S. K., & Pandit, P. V. (2023). Health Policy Implementation in Developing Nations: Challenges and Solutions. South Eastern European Journal of Public Health, 138–149. https://doi.org/10.70135/seejph.vi.447Karamagi HC, Njuguna D, Kidane SN, Djossou H, … et al.(2023). Financing health system Elements in Africa: A scoping review. PLoS One 18(9):e0291371. doi: 10.1371/journal.pone.0291371. PMID: 37703243; PMCID: PMC10499258.Kshatriya M, Syal R, Als D, Muralidharan O, Akindole B, Padhani ZA, Das J, Bhutta ZA. (2026). Implementation of health and health-related sustainable development goals: progress, challenges and opportunities-a systematic literature review update. BMJ Glob Health 11(2):e021623. doi: 10.1136/bmjgh-2025-021623. PMID: 41629068; PMCID: PMC12878203.Kutzin, J. (2013). Health financing for universal coverage and health system performance: Concepts and implications for policy. Bulletin of the World Health Organization, 91(8), 602-611.doi: 10.2471/BLT.12.113985. Epub 2013 Jun 17. PMID: 23940408; PMCID: PMC3738310.Lazo-Porras, M., & Penniecook, T. (2023). Health equity: Access to quality services and caring for underserved populations. Health Policy and Planning, 38(Suppl 2), ii1–ii2.doi: 10.1093/heapol/czad073. PMID: 37995262; PMCID: PMC10666925.Madu, A. C., & Osborne, K. (2023). Healthcare Financing in Nigeria: A Policy Review. International Journal of Social Determinants of Health and Health Services, 53(4), 434-443. doi: 10.1177/27551938231173611. Epub 2023 May 15. PMID: 37186783.Manyazewal, T. (2017). Using the World Health Organization health system building blocks Through survey of healthcare professionals to determine the performance of public healthcare facilities. Archives of Public Health, 75, 50.doi: 10.1186/s13690-017-0221-9. PMID: 29075485; PMCID: PMC5651704.Mao W, Watkins D, Sabin ML, Huang K, …et al.(2023). Effects of public financing of essential Maternal and child health interventions across wealth quintiles in Nigeria: an extended cost-effectiveness analysis. Lancet Glob Health 11(4):e597-e605. doi: 10.1016/S2214-109X(23)00056-6. PMID: 36925179; PMCID: PMC10030457.Mbachu, Chinyere, Etiaba, Enyi, Onyedinma, Chioma, Onwujekwe, Obinna & Kreling, Beth (2024). Strengthening health system resilience: lessons from Nigeria’s COVID-19 pandemic governance strategies. World Health Organization. Regional Office for Africa. https://iris.who.int/handle/10665/379804. License: CC BY-NC-SA 3.0 IGOMcKenzie, A., Sokpo, E., & Ager, A. (2014). Bridging the Policy-Implementation Gap in Federal Health Systems: Lessons from the Nigerian Experience. Journal of Public Health in Africa 5(2), 381. doi: 10.4081/jphia.2014.381. PMID: 28299131; PMCID: PMC5345418.Mishra, V. (2026). Global health systems 'at risk' as funding cuts bite, warns WHO. UN News.Retrieved from https://news.un.org/en/story/2026/02/1166869 0n 13th February, 2026Mounier-Jack, S., Griffiths, U. K., Closser, S., Burchett, H., & Marchal, B. (2014). Measuring the Health systems impact of disease control programmes: a critical reflection on the WHO building blocks framework. BMC Public Health 14, 278. doi: 10.1186/1471-2458-14-278. PMID: 24666579; PMCID: PMC3974593.National Bureau of Statistics. (2022). Nigeria Multidimensional Poverty Index Report 2022. Abuja: NBS. Retrieved from https://nigerianstat.gov.ng/pdfuploads/NIGERIA%20MULTIDIMENSIONAL%20POVERTY%20INDEX%20SURVEY%20RESULTS%202022.pdf on 13th February, 2026National Population Commission & ICF. (2024). Nigeria Demographic and Health Survey 2023.Abuja: NPC. Retrieved from https://www.health.gov.ng/wp-content/uploads/2025/10/NDHS-2024-Final-Report_Disseminated17102025.pdf on 13th February, 2026Ogunniyi, T.J. Abdulganiyu, M.O. Issa, J.B. Abdulhameed, I. Batisani, K. (2025).Ending Tuberculosis in Nigeria: a priority by 2030. BMJ Glob Health 9(12):e016820. doi: 10.1136/bmjgh-2024-016820. PMID: 39631791; PMCID: PMC11624813.Okeke, C., Onwujekwe, O., Etiaba, E., Ezenwaka, U., & Kreling, B. (2022). Essential health care service disruption due to COVID-19: lessons for sustainability in Nigeria. World Health Organization Regional Office for Africa. https://iris.who.int/handle/10665/363668.Oniyire F, Ajose T, Andu L, Adepase A, 2025). Infrastructure, service delivery, and staffing gaps In primary health care facilities in Lagos State, Nigeria: a state-wide assessment. Discover Public Health 22(1):906. doi: 10.1186/s12982-025-01321-y. PMID: 41487680; PMCID: PMC12756277.Onwujekwe, O., Ezumah, N., Mbachu, C., Obi, F., Ichoku, H., Uzochukwu, B., & Wang, H. (2019). Exploring the effectiveness of different health financing mechanisms in Nigeria: what needs to change and how can it happen? BMC Health Services Research, 19(1), 661.doi: 10.1186/s12913-019-4512-4. PMID: 31519181; PMCID: PMC6743191.Opabunmi, T., Adeyemi, D. A., Adepoju, A. G., Egboja, U., Opabunmi, O., & Adegbola, A. E. (2025). Improving access and equity in global healthcare systems: Comparing the operational insights from Nigeria and the United Kingdom. Journal of Medicine and Health Research, 10(1), 53–63.DOI: 10.56557/jomahr/2025/v10i19207Owutuamo, E. M., & Chilaka, F. C. (2025). Public Health Policy and Local Government Responses in Nigeria: Lessons from the COVID-19 Pandemic. UKR Journal of Medicine and Medical Research, 1(1), 16-31. https://ukrpublisher.com/wp-content/uploads/2025/05/UKRJMMR0305-2025.pdfPaschoalotto, M. A. C., Lazzari, E. A., Rocha, R., Massuda, A., & Castro, M. C. (2023). Health Systems resilience: is it time to revisit resilience after COVID-19? Social Science Medicine, 320, 115716. doi: 10.1016/j.socscimed.2023.115716. PMID: 36702027; PMCID: PMC9851720.Peters, D. H., & Alonge, O. (2022). Health Policy and Systems Research: The Role of Implementation Research. In S. Siddiqi, A. Mataria, K. D. Rouleau, & M. Iqbal (Eds.), Making Health Systems Work in Low and Middle Income Countries: Textbook for Public Health Practitioners (pp. 208–224). Cambridge: Cambridge University Press.Rasanathan, K. (2024). How can health systems under stress achieve universal health coverage And health equity?. Int J Equity Health 23, 244 (2024). https://doi.org/10.1186/s12939-024-02293-2Rodin, J. (2015). The Resilience Dividend. Stanford Social Innovation Review. https://doi.org/10.48558/J3QZ-5M03Siddiqi, S. Masud, T.I. Nishtar, S. Peters, D.H. Sabri, B. Bile, K.M. Jama, M.A. (2009). Framework for assessing governance of the health system in developing countries: gateway to good governance. Health Policy90(1):13-25. doi: 10.1016/j.healthpol.2008.08.005. PMID: 18838188.Topp, S. M. (2020). Power and politics: the case for linking resilience to health system governance. BMJ Global Health, 5(6), e002891.doi:10.1136/ bmjgh-2020-002891Vărzaru, A.A. (2025) Assessing the Relationships of Expenditure and Health Outcomes in Healthcare Systems: A System Design Approach. Healthcare (Basel)13(4):352. doi: 10.3390/healthcare13040352. PMID: 39997227; PMCID: PMC11855787.Wagstaff, A., Flores, G., Hsu, J., Smitz, M. F., Chepynoga, K., Buisman, L. R., & Eozenou, P. (2018). Progress on catastrophic health spending in 133 countries: A retrospective observational study. The Lancet Global Health, 6(2), e169-e179. doi: 10.1016/S2214-109X(17)30429-1. PMID: 29248367.Welcome MO. (2011). The Nigerian health care system: Need for integrating adequate medical Intelligence and surveillance systems. Jourbal of Pharmacy Bioallied Sciences 4:470-8. doi: 10.4103/0975-7406.90100. PMID: 22219580; PMCID: PMC3249694.Witter S, Thomas S, Topp SM, Barasa E, Chopra M, Cobos D, Blanchet K, Teddy G, Atun R, Ager A. (2023). Health system resilience: a critical review and reconceptualisation. Lancet Glob Health 11(9):e1454-e1458. doi: 10.1016/S2214-109X(23)00279-6. PMID: 37591591.World Health Organization. (2007). Everybody's business: strengthening health systems to Improve health outcomes: WHO's framework for action. Geneva: WHO. Retrieved from https://www.who.int/publications/i/item/everybody-s-business----strengthening-health-systems-to-improve-health-outcomes on 13th February, 2026World Health Organization. (2023b). Health Systems Resilience. Geneva: WHO. Retrieved from https://www.who.
Downloads
Published
Issue
Section
Categories
License
Copyright (c) 2026 Ismail Tukur, Bello Almu, Tijjani Suleman, Shafiu Dauda, Jamilu Umar Gora

This work is licensed under a Creative Commons Attribution 4.0 International License.




